Contents
Healthcare is on the brink of a significant transformation, driven by technological advancements that promise to enhance patient care and outcomes. One of the most compelling innovations is non-invasive glucose monitoring, which offers a way to track blood sugar levels without the discomfort of traditional methods. This shift not only improves the user experience but also has the potential to revolutionize diabetes management. The challenge lies in effectively implementing these technologies to ensure accuracy, reliability, and user engagement.
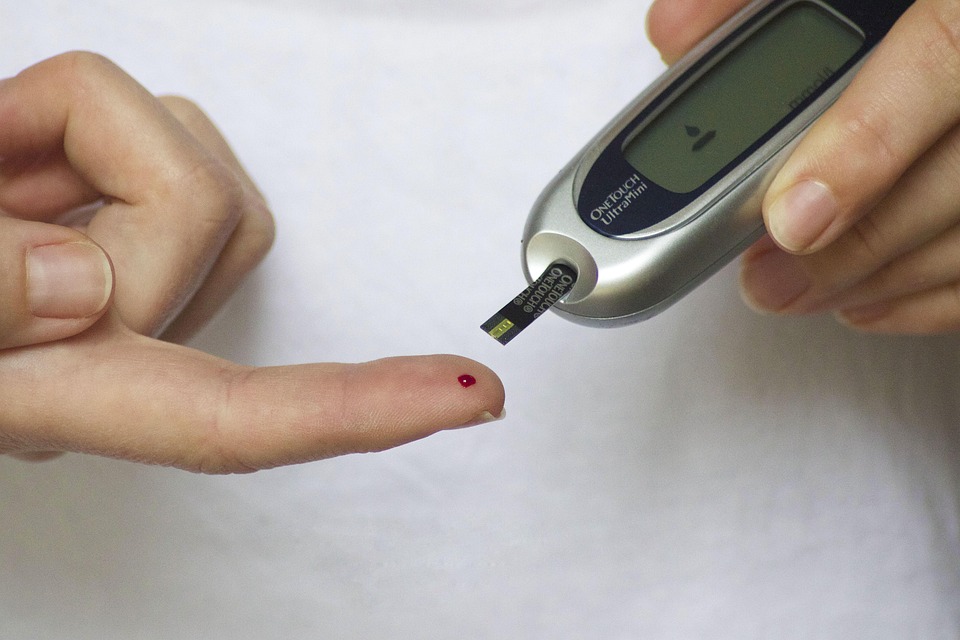
The traditional methods of glucose monitoring often involve finger pricks that can lead to discomfort and non-compliance among patients. A non-invasive approach eliminates this barrier, allowing for continuous monitoring without the pain associated with conventional methods. This is particularly crucial for individuals with diabetes who require frequent checks throughout the day. However, the technology must be robust enough to provide real-time, accurate data that users can trust.
As the demand for wearable health technology grows, the market for non-invasive glucose monitoring devices is expanding rapidly. Companies are investing heavily in research and development to create devices that are not only effective but also user-friendly. The integration of these devices into healthcare systems requires careful planning and execution to maximize their benefits. Understanding the technical aspects and potential pitfalls is essential for successful implementation.
With the right strategies in place, non-invasive glucose monitoring can significantly improve health outcomes and patient satisfaction. This guide aims to provide a comprehensive overview of how to effectively implement these technologies, common pitfalls to avoid, and the technical frameworks that support them. By leveraging the insights provided, healthcare providers and technology developers can work together to create a future where diabetes management is more accessible and less invasive.
How to Implement Non-Invasive Glucose Monitoring for Real Results
- Best Tool: Continuous Glucose Monitoring System (CGM)
- Optimal Configuration: Set the sensor calibration frequency to every 12 hours for maximum accuracy.
- Expected Outcome: Achieve a 20% reduction in hypoglycemic events within three months.
Preparation for Implementation
Before deploying non-invasive glucose monitoring systems, healthcare providers must assess their current infrastructure and patient needs. This involves evaluating existing patient management systems and determining how new data will integrate into these systems. A thorough understanding of patient demographics and their specific health challenges is crucial. Additionally, training staff on how to use and interpret data from these devices will enhance their effectiveness. Engaging patients early in the process can also foster acceptance and compliance.
Choosing the right technology is another critical step. Various devices on the market offer different features, such as Bluetooth connectivity, real-time alerts, and data analytics capabilities. Selecting a device that aligns with the specific needs of the patient population is essential. Conducting pilot tests with a small group of patients can provide valuable insights into usability and effectiveness. This step helps identify any potential issues before a full-scale rollout.
Establishing partnerships with technology providers can streamline the implementation process. Collaborating with companies that specialize in non-invasive glucose monitoring can provide access to the latest innovations and technical support. These partnerships can also facilitate data sharing, which is vital for comprehensive patient management. Ensuring that all stakeholders are aligned on goals and expectations will contribute to a smoother implementation process. Regular feedback loops can help refine the approach as needed.
Pro Tip: Always involve patients in the selection process to ensure the technology meets their needs and preferences.
Action Steps for Deployment
Once the groundwork is laid, the next step is to deploy the non-invasive glucose monitoring systems. This process should begin with a clear communication strategy to inform patients about the new technology and its benefits. Providing educational resources, such as tutorials and FAQs, can help patients feel more comfortable with the transition. Additionally, establishing a support system for troubleshooting issues can enhance patient satisfaction and adherence to the new monitoring protocols.
Data management is another critical aspect of deployment. Ensuring that data collected from glucose monitoring devices is securely stored and easily accessible is paramount. Implementing robust data encryption protocols can protect patient information while allowing healthcare providers to analyze trends effectively. Utilizing cloud-based solutions can facilitate real-time data access and sharing among healthcare teams. Regular system audits can help identify any vulnerabilities in data security.
Monitoring the effectiveness of the implementation is essential for continuous improvement. Setting clear metrics for success, such as patient engagement rates and health outcomes, allows for ongoing evaluation. Regularly reviewing this data can help identify areas for improvement and inform future strategies. Engaging patients in feedback sessions can provide insights into their experiences and highlight any challenges they face. This iterative process ensures that the technology remains effective and relevant to patient needs.
Pro Tip: Use patient feedback to refine educational materials and support resources continuously.
User Experience Optimization
Optimizing the user experience is vital for the success of non-invasive glucose monitoring systems. The design of the device should prioritize comfort and ease of use, ensuring that patients can wear it without discomfort. User interface design should be intuitive, allowing patients to easily navigate features and access their data. Regular updates to the software can enhance usability and introduce new features based on user feedback. Ensuring that the device is aesthetically pleasing can also improve patient acceptance.
Incorporating gamification elements can further enhance user engagement. Features such as rewards for consistent monitoring or educational quizzes can motivate patients to adhere to their monitoring routines. These elements can create a more enjoyable experience, making patients more likely to use the technology regularly. Providing personalized insights based on their data can also increase engagement, as patients can see the direct impact of their monitoring on their health.
Ensuring seamless integration with other health applications can enhance the overall user experience. Many patients use multiple health tracking apps, and allowing data synchronization can provide a more comprehensive view of their health. This integration can lead to more informed decision-making and improved health outcomes. Regularly updating users on new features and improvements can keep them engaged and informed about the technology’s evolution.
Pro Tip: Regularly solicit user feedback to identify areas for improvement in the user experience.
Common Configuration Risks
Inadequate Calibration Protocols
One common error in implementing non-invasive glucose monitoring systems is inadequate calibration protocols. Many devices require regular calibration to maintain accuracy, and failing to establish a clear schedule can lead to erroneous readings. This can result in poor patient outcomes, as users may make decisions based on inaccurate data. Implementing a strict calibration schedule, such as every 12 hours, can mitigate this risk. Regular training for staff on calibration procedures is also essential to ensure compliance.
Another risk associated with calibration is the potential for user error. Patients may not understand the importance of calibration or how to perform it correctly. Providing clear instructions and visual aids can help alleviate this issue. Additionally, incorporating reminders within the device’s software can prompt users to calibrate at the appropriate times. Monitoring compliance with calibration protocols can help identify any issues early on.
Data Security Vulnerabilities
Data security is a critical concern in the deployment of non-invasive glucose monitoring systems. Many devices collect sensitive patient information, making them attractive targets for cyberattacks. Failure to implement robust security measures can lead to data breaches, compromising patient confidentiality. Utilizing industry-standard encryption protocols, such as AES-256, can help protect data during transmission and storage. Regular security audits can identify vulnerabilities and ensure compliance with data protection regulations.
Another aspect of data security involves ensuring that all personnel handling patient data are adequately trained. Staff should be aware of best practices for data handling and the importance of maintaining confidentiality. Implementing role-based access controls can limit data access to authorized personnel only. Regular training sessions can reinforce these practices and keep staff updated on emerging threats.
Integration Challenges with Existing Systems
Integrating non-invasive glucose monitoring systems with existing healthcare infrastructure can present significant challenges. Many healthcare organizations use legacy systems that may not be compatible with new technologies. This can lead to data silos, where valuable information is not shared across platforms. Conducting a thorough assessment of existing systems before implementation can help identify potential integration issues. Working closely with technology providers can facilitate smoother integration processes.
Another challenge is ensuring that all stakeholders are aligned on integration goals. Miscommunication can lead to delays and frustration among staff and patients. Establishing clear lines of communication and regular check-ins can help keep everyone informed and engaged. Creating a dedicated project team to oversee the integration process can also enhance accountability and streamline efforts.
The Architecture of Non-Invasive Monitoring Systems
The architecture of non-invasive glucose monitoring systems is built on several key protocols and standards that ensure accuracy and reliability. One of the primary protocols is ISO 15197, which outlines the requirements for blood glucose monitoring systems. Adhering to this standard ensures that devices provide accurate and reliable measurements, which is crucial for effective diabetes management. Regular compliance checks against this standard can help maintain device integrity.
Another important standard is the Health Level Seven (HL7) protocol, which facilitates the exchange of health information between different systems. Implementing HL7 ensures that data from glucose monitoring devices can be integrated seamlessly into electronic health records. This integration is vital for comprehensive patient management and allows healthcare providers to make informed decisions based on real-time data. Regular updates to HL7 standards can enhance interoperability and data sharing capabilities.
Security protocols, such as the Health Insurance Portability and Accountability Act (HIPAA), are also critical in the architecture of these systems. Compliance with HIPAA ensures that patient data is protected and that healthcare organizations are held accountable for data breaches. Regular training on HIPAA compliance for all staff members can help mitigate risks associated with data handling. For further insights on the importance of these standards, refer to Source Evidence.
Choosing the Right Solution
- Assess Compatibility: Ensure that the device is compatible with existing health management systems to avoid integration issues. This compatibility will streamline data sharing and enhance patient management.
- Evaluate User Experience: Prioritize devices that offer an intuitive user interface and comfort for patients. A positive user experience can lead to higher adherence rates and better health outcomes.
- Consider Data Security: Opt for solutions that adhere to industry-standard security protocols to protect patient information. Implementing robust security measures is essential for maintaining patient trust and compliance.
Pros & Cons
| The Benefits | Potential Downsides |
|---|---|
| Improved patient compliance due to reduced discomfort. | Initial costs can be high for advanced technology. |
| Real-time data allows for proactive health management. | Potential data security vulnerabilities if not properly managed. |
| Enhanced patient engagement through user-friendly interfaces. | Integration challenges with existing healthcare systems may arise. |
Tools and Workflows
Implementing non-invasive glucose monitoring systems can be enhanced by utilizing complementary tools. Integrating data analytics platforms can provide deeper insights into patient trends and behaviors. Using mobile health applications can facilitate communication between patients and healthcare providers, allowing for timely interventions. Regular training on these tools can ensure that staff are equipped to leverage the full potential of the technology.
Who Should Avoid This?
Individuals with certain medical conditions or those who are pregnant should consult with healthcare providers before using non-invasive glucose monitoring systems. These devices may not provide accurate readings for all users, particularly in cases of fluctuating blood sugar levels. Additionally, patients with skin sensitivities may experience discomfort from wearing monitoring devices. A thorough assessment by a healthcare professional can help determine the best monitoring approach for each individual.
Common Questions
What is non-invasive glucose monitoring?
This technology allows users to monitor their blood sugar levels without the need for finger pricks. It typically uses sensors placed on the skin to measure glucose levels continuously.
How accurate are non-invasive glucose monitors?
Accuracy can vary by device, but many are designed to meet industry standards for glucose monitoring. Regular calibration and proper use are essential for maintaining accuracy.
Can non-invasive glucose monitors replace traditional methods?
While they offer significant advantages, non-invasive monitors may not completely replace traditional methods for all patients. Consulting with healthcare providers is crucial for determining the best approach.
The Bottom Line
Non-invasive glucose monitoring presents a transformative opportunity in diabetes management. By implementing the right strategies and technologies, healthcare providers can enhance patient care and outcomes.
- Focus on user experience to improve compliance.
- Ensure robust data security measures are in place.
- Regularly evaluate and refine implementation strategies.