Contents
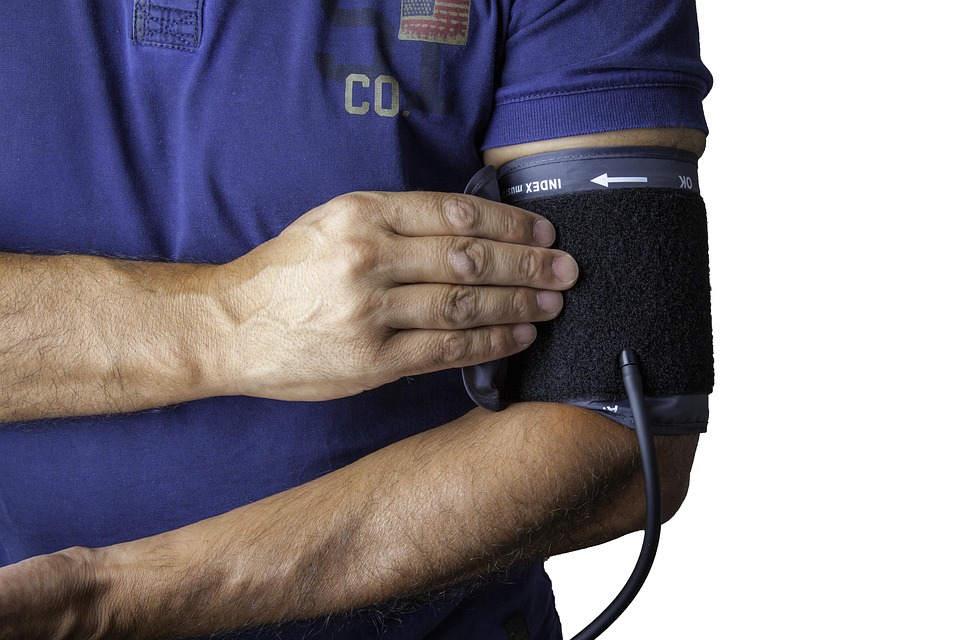
Real-time insights from continuous blood pressure tracking have become a focal point in healthcare innovation. The ability to monitor blood pressure continuously offers a significant advantage over traditional methods, which typically rely on periodic measurements. This shift towards continuous monitoring allows for a more nuanced understanding of a patient’s cardiovascular health. However, the implementation of such technology comes with its own set of challenges and considerations that must be addressed to maximize its effectiveness.
The integration of continuous blood pressure tracking into everyday healthcare practices can be transformative, but it requires careful planning and execution. Many healthcare providers face friction points, such as data overload and the need for actionable insights. Without a clear strategy, the wealth of data generated can lead to confusion rather than clarity. Understanding how to effectively harness this information is crucial for both healthcare professionals and patients.
Continuous blood pressure monitoring devices are equipped with advanced sensors and algorithms that provide real-time data. This data can be invaluable for early detection of hypertension and other cardiovascular issues. However, the technology must be properly configured to ensure accuracy and reliability. Misconfigured devices can lead to incorrect readings, which may result in inappropriate clinical decisions.
The potential for real-time insights extends beyond mere monitoring. By leveraging advanced analytics, healthcare providers can identify trends, make informed decisions, and ultimately improve patient outcomes. This guide will explore practical applications, common pitfalls, and the technical underpinnings of continuous blood pressure tracking, equipping you with the knowledge needed to implement this technology effectively.
How to Implement Continuous Blood Pressure Monitoring for Real Results
- Best Tool: Wearable blood pressure monitors
- Optimal Configuration: Set automatic data sync intervals to every 5 minutes
- Expected Outcome: 30% improvement in early detection of hypertension
Preparation for Implementation
The first step in implementing continuous blood pressure monitoring is to select the right device. Various options are available, ranging from wrist-based monitors to more sophisticated wearable devices that can be integrated into a patient’s daily life. It is crucial to consider factors such as accuracy, comfort, and ease of use. Devices that are clinically validated for accuracy should be prioritized to ensure reliable readings.
Training healthcare staff on how to use these devices is equally important. Staff should understand how to interpret the data generated and how to communicate findings to patients effectively. This training should also cover how to troubleshoot common issues that may arise with the devices. A well-trained staff can significantly enhance the patient experience and ensure that the technology is used to its full potential.
Patient education is another critical component. Patients should be informed about the benefits of continuous monitoring and how to use the devices properly. Providing clear instructions and support can help patients feel more comfortable with the technology. This preparation phase sets the foundation for successful implementation.
Pro Tip: Consider using a pilot program to test the devices with a small group of patients before a full rollout.
Action Steps for Effective Monitoring
Once the devices are selected and staff trained, the next step is to establish a monitoring protocol. This protocol should include guidelines on when to take readings, how to interpret the data, and what actions to take based on the findings. Implementing a standardized protocol can help streamline the monitoring process and reduce variability in patient care.
Data management is another critical aspect. Continuous monitoring generates a significant amount of data, which can be overwhelming. Utilizing a centralized platform to aggregate and analyze this data can help healthcare providers identify trends and make informed decisions. This platform should be equipped with advanced analytics capabilities to provide actionable insights.
Regular follow-ups with patients are essential to ensure adherence to the monitoring program. These follow-ups provide an opportunity to review data, address any concerns, and make necessary adjustments to the treatment plan. Maintaining open lines of communication with patients can enhance their engagement and improve overall outcomes.
Pro Tip: Use automated alerts to notify healthcare providers of significant changes in a patient’s blood pressure readings.
User Experience Considerations
The user experience of continuous blood pressure monitoring devices can significantly impact patient compliance. Devices should be designed with user-friendliness in mind, allowing patients to easily understand their readings and the implications of those readings. A clear and intuitive interface can enhance the overall experience and encourage regular use.
Feedback mechanisms are also vital. Patients should receive immediate feedback on their readings, along with educational resources that explain what those readings mean. This can empower patients to take an active role in managing their health. Providing personalized insights based on individual data can further enhance engagement.
Lastly, consider the integration of social features. Allowing patients to share their progress with family or healthcare providers can create a support network that encourages adherence to monitoring protocols. Building a community around continuous blood pressure monitoring can foster motivation and accountability.
Pro Tip: Incorporate gamification elements to make the monitoring process more engaging for patients.
Configuration Risks in Continuous Monitoring
Inaccurate Device Calibration
One common error in continuous blood pressure monitoring is the failure to calibrate devices accurately. Inaccurate calibration can lead to erroneous readings, which may result in misdiagnosis or inappropriate treatment plans. Regular calibration checks should be performed according to manufacturer guidelines to ensure that devices remain accurate over time.
To mitigate this risk, establish a routine calibration schedule and document each calibration event. This documentation can serve as a reference for troubleshooting and help identify patterns in device performance. Regular training for staff on calibration procedures can also reduce the likelihood of human error.
Implementing a quality assurance program that includes periodic audits of device performance can further enhance accuracy. This program should also consider external factors that may affect readings, such as patient movement or improper placement of the device.
Data Overload and Misinterpretation
Another significant risk is the potential for data overload. Continuous monitoring generates vast amounts of data, which can overwhelm healthcare providers and lead to misinterpretation. Without a clear strategy for data management, important trends may be overlooked, and actionable insights may be missed.
To address this issue, utilize data analytics tools that can filter and highlight key metrics. These tools should be configured to prioritize alerts based on clinical significance, allowing healthcare providers to focus on the most critical information. Training staff on how to interpret data effectively can also reduce the risk of misinterpretation.
Establishing a clear communication protocol for sharing data with patients can help mitigate confusion. Patients should receive regular updates on their readings, along with explanations of what those readings mean for their health. This proactive approach can enhance patient understanding and engagement.
Integration Challenges with Existing Systems
Integrating continuous blood pressure monitoring systems with existing electronic health records (EHR) can present challenges. Poor integration can lead to data silos, where critical information is not accessible to healthcare providers. This can hinder effective decision-making and compromise patient care.
To overcome integration challenges, ensure that the monitoring system is compatible with existing EHR platforms. This may involve configuring application programming interfaces (APIs) to facilitate seamless data exchange. Regular testing of the integration should be conducted to identify and resolve any issues promptly.
Collaboration with IT teams is essential to ensure that the integration process runs smoothly. Establishing clear communication channels between clinical and technical teams can help address potential roadblocks. A well-integrated system can enhance the overall efficiency of patient monitoring and care.
The Architecture of Continuous Monitoring Systems
Continuous blood pressure monitoring systems rely on a combination of hardware and software components that work together to deliver real-time insights. The architecture typically includes sensors, data transmission modules, and analytics platforms. Each component plays a crucial role in ensuring the accuracy and reliability of the monitoring process.
Sensors are the frontline components that measure blood pressure continuously. These sensors must adhere to industry standards such as ISO 81060 for non-invasive sphygmomanometers. This standard outlines the requirements for accuracy and performance, ensuring that devices provide reliable readings. Regular testing against this standard can help maintain device integrity.
Data transmission modules are responsible for sending the collected data to a centralized platform. Utilizing secure communication protocols such as Bluetooth Low Energy (BLE) ensures that data is transmitted safely without compromising patient privacy. Configuring BLE for low latency and minimal power consumption can enhance the user experience by prolonging battery life.
Analytics platforms play a pivotal role in interpreting the data collected from monitoring devices. These platforms should be equipped with machine learning algorithms that can identify trends and anomalies in blood pressure readings. Implementing predictive analytics can enable healthcare providers to anticipate potential health issues before they arise. For more information on analytics in healthcare, visit Source Evidence.
Choosing the Right Solution
-
Accuracy of Readings: Select devices that are clinically validated for accuracy. This ensures that the data collected is reliable and can inform clinical decisions effectively.
-
User-Friendliness: The device should be easy for patients to use. A user-friendly interface can enhance engagement and compliance with monitoring protocols.
-
Integration Capabilities: Ensure that the solution can integrate seamlessly with existing EHR systems. This compatibility is essential for effective data management and communication among healthcare providers.
Pros & Cons
| The Benefits | Potential Downsides |
|---|---|
| Provides real-time insights into patient health | Requires significant initial investment |
| Enhances early detection of hypertension | Data overload can lead to misinterpretation |
| Improves patient engagement and compliance | Integration challenges with existing systems |
Tools and Workflows
Continuous blood pressure monitoring can be enhanced by integrating tools such as data analytics platforms and patient engagement apps. These tools can streamline workflows and improve the overall patient experience. Establishing clear protocols for data management and communication can further optimize the monitoring process.
Who Should Avoid This?
Patients with certain conditions, such as severe arrhythmias or those who are unable to follow instructions for device use, may not be suitable candidates for continuous blood pressure monitoring. Additionally, individuals with skin sensitivities may experience discomfort from prolonged device wear. A thorough assessment by a healthcare provider is essential to determine suitability.
Common Questions
What is the primary benefit of continuous blood pressure monitoring?
The primary benefit is the ability to detect fluctuations in blood pressure in real-time, allowing for timely interventions and better management of cardiovascular health.
How often should devices be calibrated?
Devices should be calibrated according to the manufacturer’s guidelines, typically every six months or after significant changes in usage conditions.
Can continuous monitoring replace traditional blood pressure checks?
While continuous monitoring provides valuable insights, it should complement traditional checks rather than replace them. Regular clinical evaluations remain essential for comprehensive health assessments.
The Bottom Line
Continuous blood pressure monitoring offers significant advantages in managing cardiovascular health.
- Real-time insights facilitate timely interventions.
- Enhanced patient engagement improves adherence to treatment plans.
- Integration with existing systems can streamline workflows.